|
|
The Gladden Society presents its inaugural JRGOS CASE CORNER submitted by Christian Pean, MD, Gladden Member and Orthopaedic Trauma and Reconstruction Surgeon, Core Faculty Member Duke Margolis Center for Health Policy.
CASE PRESENTATION
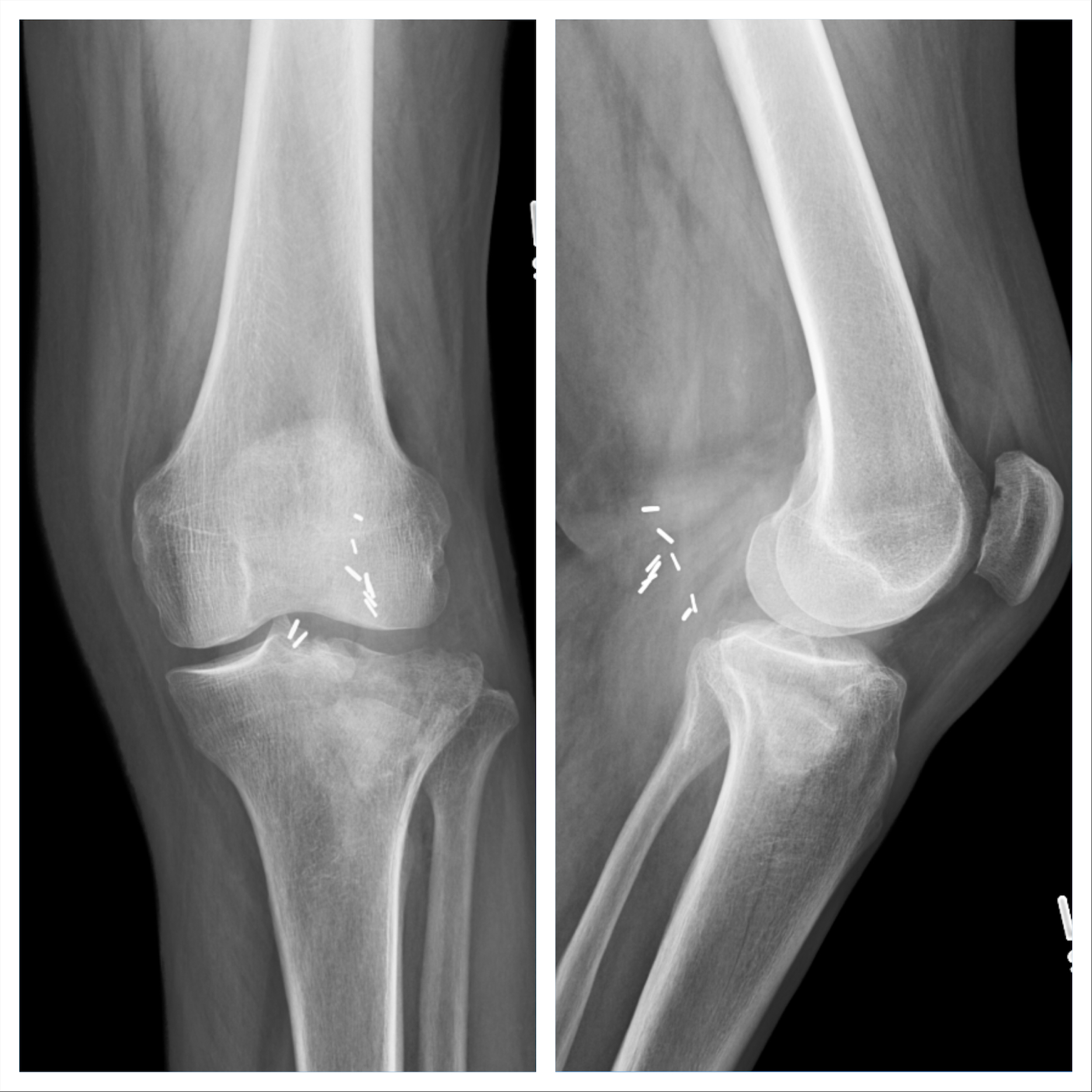
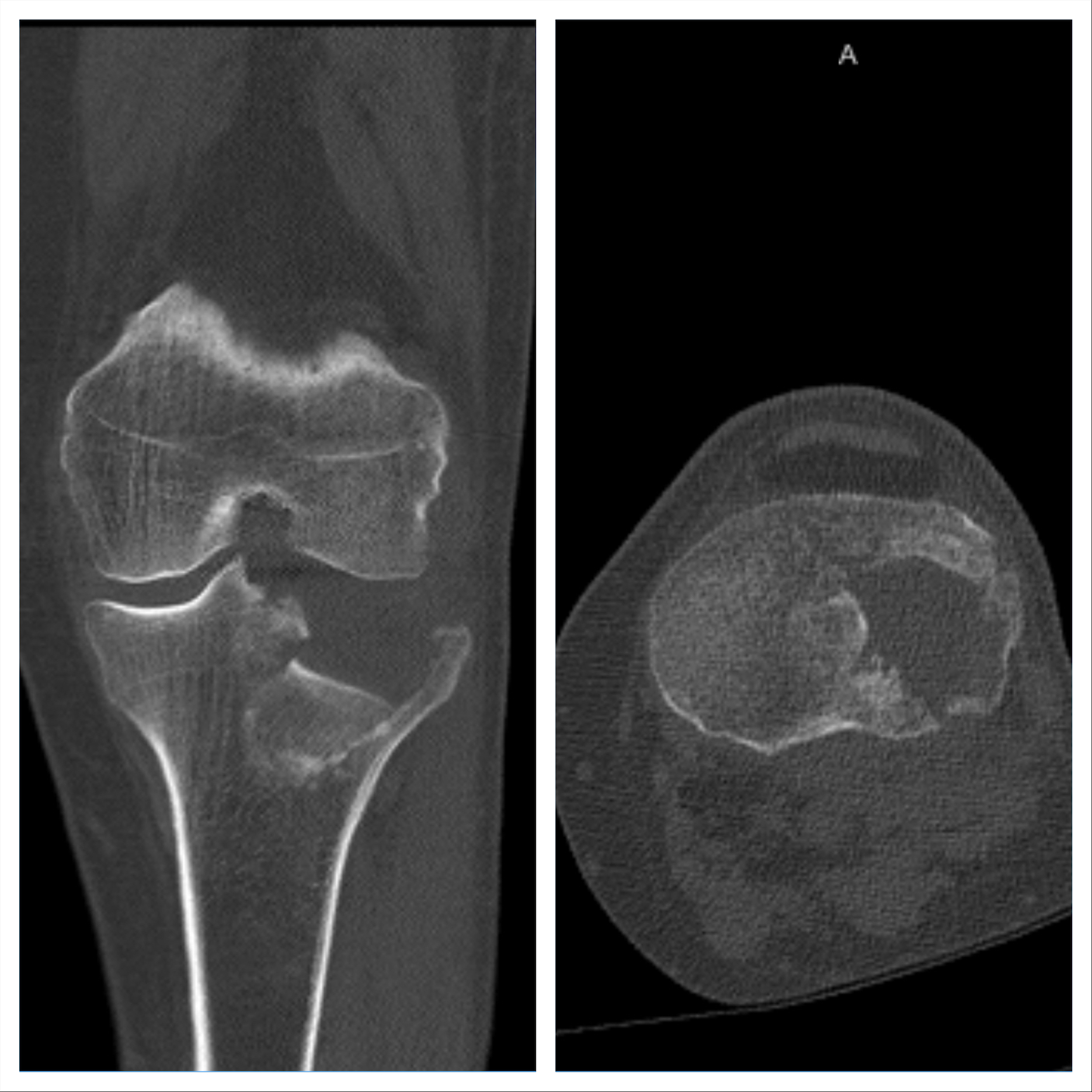
70-year-old male history of previous left knee posterior aneurysm with subsequent repair—otherwise healthy, sustained left split depression tibial plateau fracture after a twisting fall from a ladder. This patient presented 3 weeks after his initial injury. On exam his skin is intact, minimal swelling is appreciated, and he has ttp about the knee with the knee caving in on valgus stress. He’s neurovascularly intact. Imaging further demonstrates the severe posterolateral depression of the tibial plateau articular surface from the femur’s initial impact during injury.
DIAGNOSIS
Schatzker 2 Tibial Plateau Fracture
|
|
|
HOT TIPS
- Greater than 10mm of tibial plateau articular surface depression correlates with a high concomitant lateral meniscus tear, thus a submeniscal arthrotomy both for joint surface evaluation as well as possible meniscus tear is warranted
- ALIGNMENT rather than articular restoration is a key factor associated with posttraumatic arthritis
- 20-30% of tibial plateau fracture patients will develop posttraumatic arthritis, 3-7% of tibial plateau fracture patients go on to total knee arthroplasty
- Why calcium phosphate cement? A study by Lobenhoffer et al noted improved radiographic outcomes and earlier weightbearing with usage of calcium phosphate cement. Welch and Zhang reproduced tibial plateau fractures in goats and compared cancellous autograft to calcium phosphate cement augmentation. At 24 hours, four of five specimens treated with autograft had subsidence of the fragment. Only two specimens from limbs treated with cement showed minimal subsidence; the remaining were congruent. Calcium phosphate>>calcium sulfate as calcium sulfate does not have the same compressive strength, resorbs quickly, and is associated with wound drainage.
|
| TREATMENT PLAN
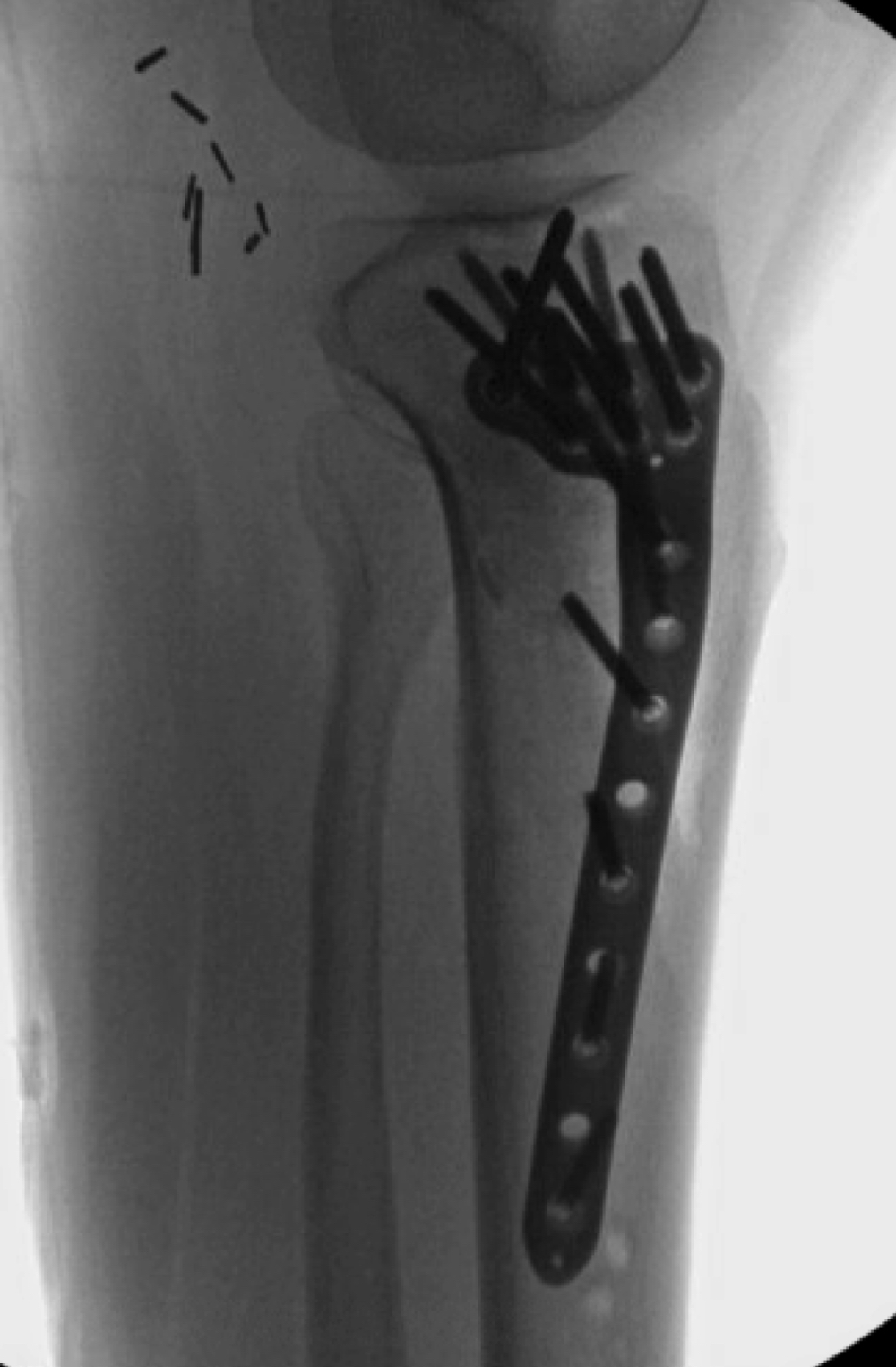
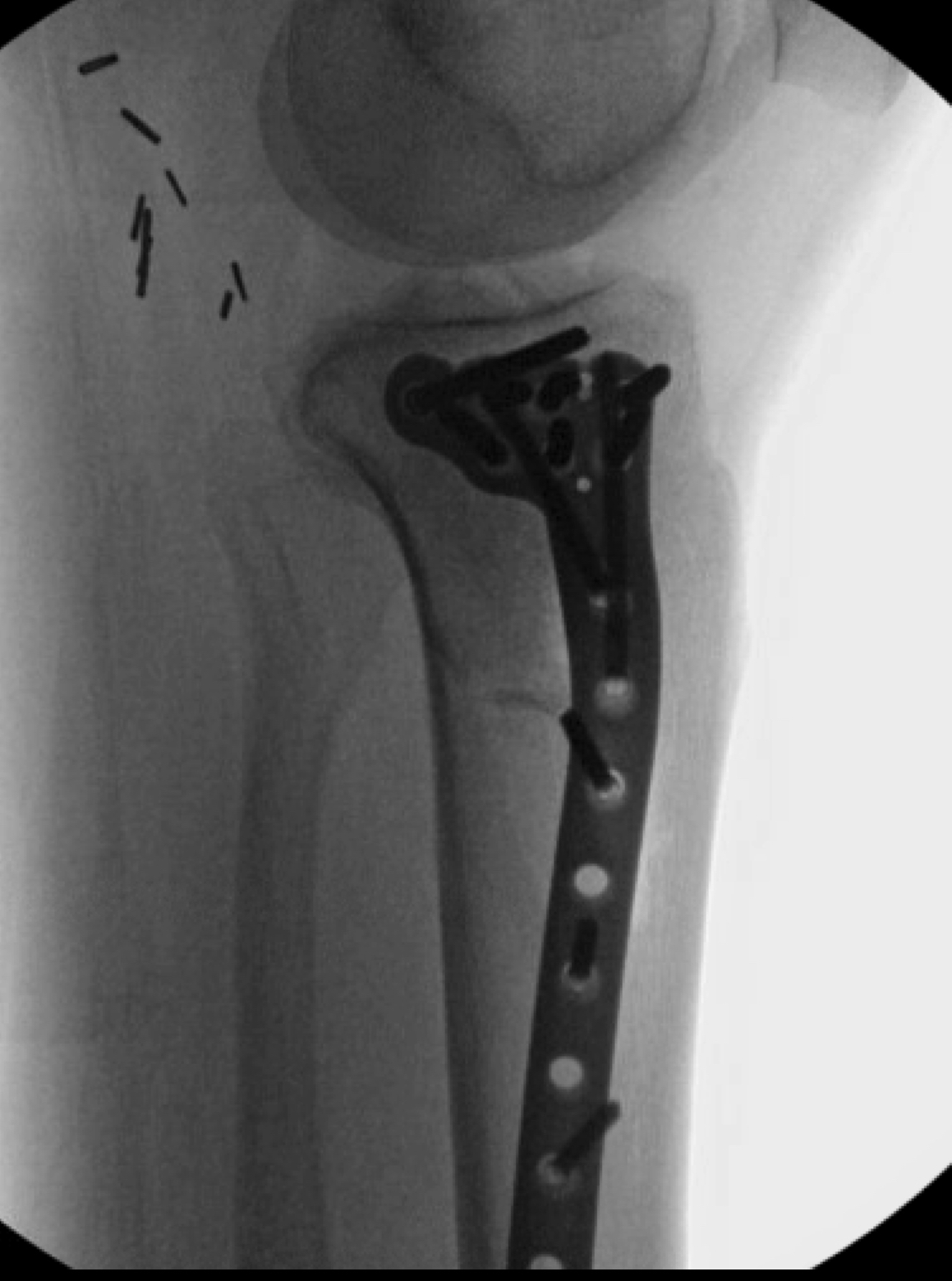
Surgery in this case consisted of open reduction internal fixation with an AO distractor to aid articular surface visualization and facilitate fracture reduction and fixation. As a partial articular pattern, this fracture is appropriate for Buttress plating, which we accomplished here using a 3.5mm proximal tibia locking plate. I opted for a locking plate in this case given there is a short segment for fixation and the patient had osteoporotic bone. To address the large void from the impaction, I used cancellous chips and calcium phosphate cement. The post op plan for this patient is non weight bearing for 10-12 weeks with immediate range of motion encouraged.
|
 |
 |
 |
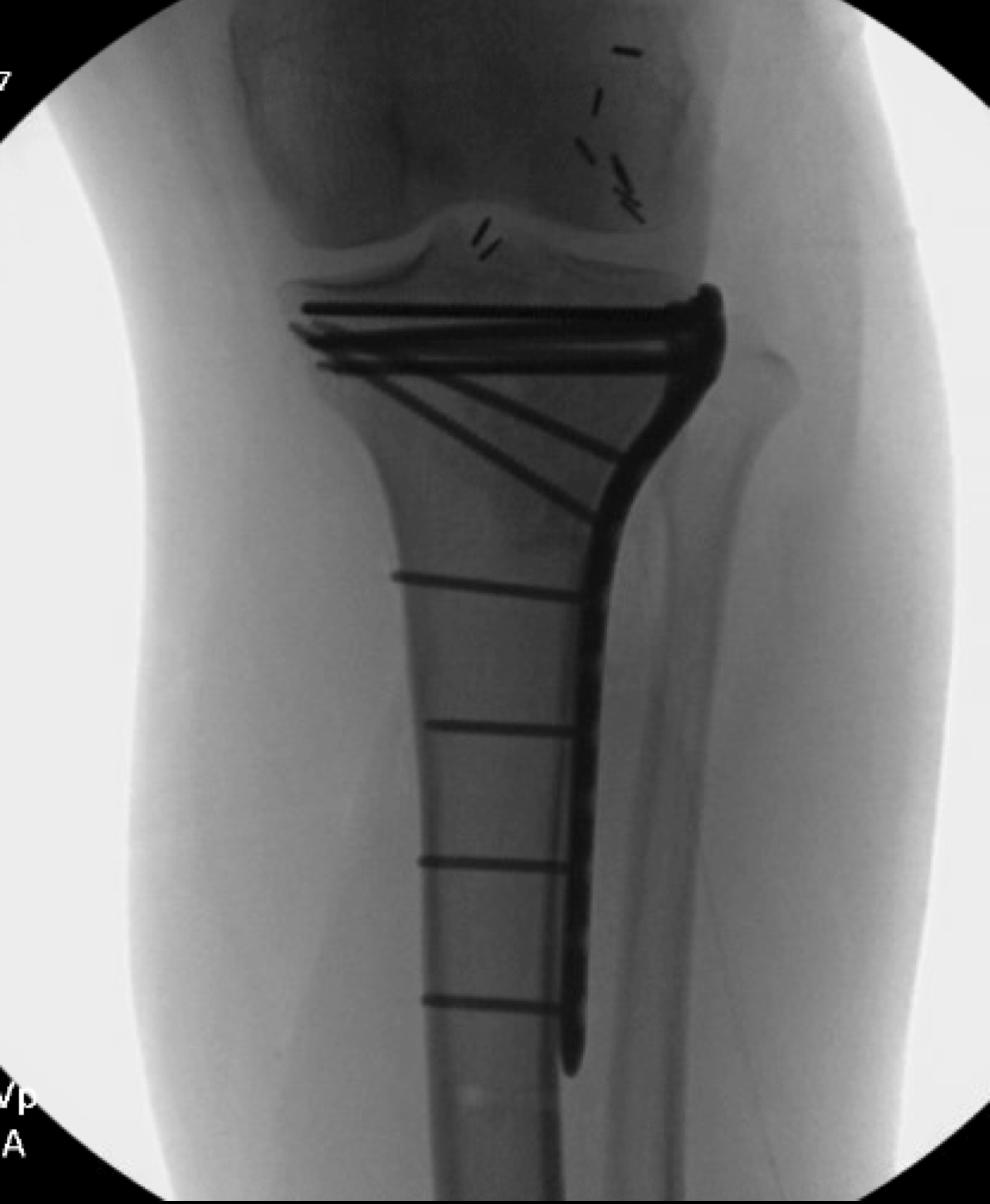 |
Implants: Zimmer ALPS 3.5mm proximal tibia plate, cancellous chips, and injectable calcium phosphate cement. Synthes AO Distractor
FOLLOW DR. PEAN ON SOCIAL MEDIA
https://www.linkedin.com/in/christianpean
https://www.instagram.com/dr.christian.pean/
https://twitter.com/DrChristianPean
|
|